Caregiving in America: The Strain, the Pain, the Emotional Drain
Eye-opening findings from a new survey of the nation's caregivers
Former First Lady Rosalynn Carter famously said: There are only four kinds of people in the world — those who have been caregivers, those who are currently caregivers, those who will be caregivers and those who will need caregivers.

The new, mammoth Caregiving in the U.S. 2020 report from AARP and the National Alliance for Caregiving (NAC) has a piercing message about the 53 million Americans who are currently family caregivers: The job is not only often tough, it’s tougher than what the researchers found in their 2015 report. Family caregivers are in worse health than they were five years ago, according to AARP and NAC.
“What we’re seeing with the caregiving report is the profile of families who take on caregiving is changing, with a shift toward more complex roles and responsibilities,” said Lynn Friss Feinberg, senior strategic policy advisor at the AARP Public Policy Institute.
Growing Numbers of Family Caregivers
Based on its survey of 1,392 caregivers (61% women; average age: 49; providing 24 hours of care weekly), AARP and NAC say that roughly 21% of Americans are caregivers. And the number of those providing caregiving for people 50 and older (41.8 million) has risen about 20% since 2015.
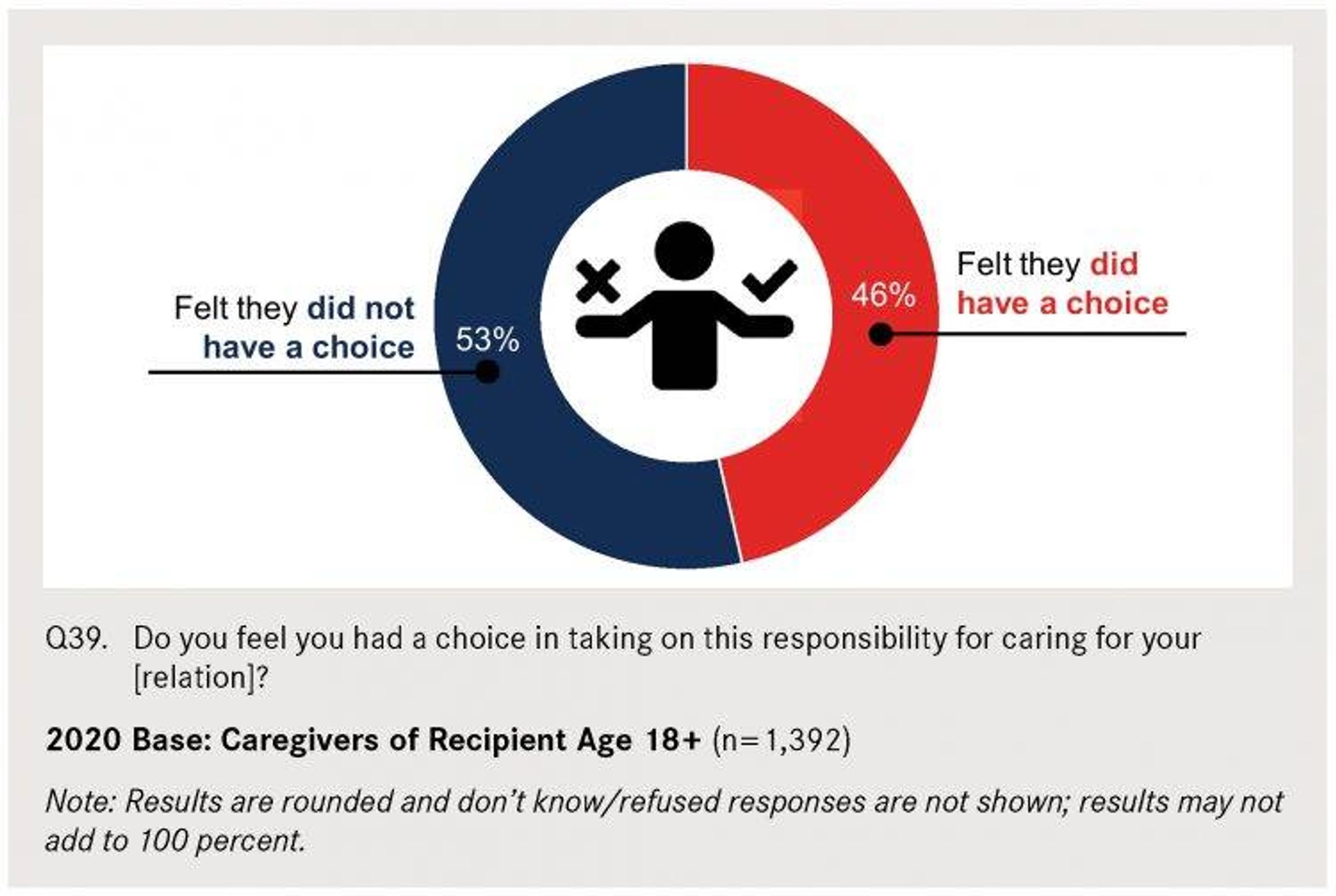
A full 66% of respondents assisting a spouse or partner said they had no choice but to provide caregiving.
“It’s not just that more people are caregiving. That makes sense as America gets older,” said C. Grace Whiting, NAC’s president and CEO. “It’s that people who are doing it are doing it for longer and are more likely to be caring for people who have multiple care needs.”
The report’s compelling statistics paint a portrait of family caregivers who are frequently feeling emotional strain, financial strain and physical strain due to the assistance they’re providing. Especially difficult: caring for a loved one with dementia. “It’s like caregiving on steroids,” said Amy Goyer, AARP’s family and caregiving expert and author of Juggling Life, Work & Caregiving.
A full 66% of respondents assisting a spouse or partner said they had no choice but to provide caregiving. Those caring for spouses or partners, as well as ones with incomes under $50,000, were the most likely to describe caregiving as high intensity.
The Coronavirus Pandemic and Caregivers
And the survey was conducted before the coronavirus pandemic began. Its researchers think caregivers would report even more economic and emotional stresses due to the coronavirus.
“The impact on [caregiving] families now with COVID is a serious and heartbreaking issue,” said Feinberg. “The financial strain, emotional strain and physical health impacts we see as a result of caregiving have been exacerbated by COVID-19.”
Added Whiting: “I think the pandemic has pulled back the curtain and brought to the forefront issues that caregivers are having.”
Despite the hardships, 51% of the caregivers surveyed said the help they’re offering “gives them a sense of purpose or meaning.” That’s even truer for Hispanic caregivers and African American caregivers; 61% and 59% of them, respectively, felt that way. Yet they were more likely than white caregivers to report that their caregiving duties are high intensity and have had deleterious financial impacts on them.
AARP’s Goyer said the survey’s findings resonated with her. She offered caregiving help to her grandparents while in her 20s and to her late mother and father (quitting her full-time AARP job and moving cross-country to do so). These days, she’s assisting her sister, who is dealing with serious health issues.
The COVID-19 restrictions on family caregivers have especially taken a toll on Goyer. “I can’t even go into a doctor’s office with my sister now,” she said. “They only allow the patient to come in, unless the patient can’t walk. That’s very frustrating. She [her sister] wants me there.”
And Goyer worries what would happen if her sister was hospitalized during the pandemic and caregivers were prohibited. “I wouldn’t be able to be there for her,” she said.
How Caregiving Impacts the Health of the Caregivers
One of the saddest findings in the Caregiving in America 2020 report, I think, is what caregiving is doing to the health of the family caregivers.
Fewer caregivers than in 2015 described their health status as excellent or very good (41%, down from 48%) and more called it fair or poor (21%, up from 17%). About one in five said caregiving has made their own health worse. “The stress associated with caregiving may exacerbate declines in health that occur with age,” the report’s authors wrote.
Goyer can relate. “When my parents moved back in with me so I could provide caregiving for them, my back went out. I hadn’t had back problems for ten years. It was clearly stress,” she said. “Eventually, my immune system was affected.”
Sherri Snelling, a corporate gerontologist who is CEO of Caregiving Club (a company that supports family caregivers), said the COVID-19 pandemic may be offering an unseen benefit for family caregivers who haven’t been taking care of themselves. “I think it’s putting self-care on center stage,” she said.
Snelling recently started sending out Caregiver Monday self-care health and wellness tips for workers who are also family caregivers. She hopes the advice “becomes a weekly routine, so you are thinking about your health as a piece of caregiving, which is so critical.”
Only 9% of employers surveyed for that study said caregiving was among their Top 5 priorities for employee health and benefit issues.
Holding a Job and Doing Caregiving on the Side
Most family caregivers surveyed said they also have full-time or part-time jobs. But only about 53% of those said their supervisor was aware of their caregiving responsibility. “You don’t want to be seen as a ‘lesser than’ employee when you have caregiving needs,” said Snelling.
And 61% of caregivers with paying jobs say that helping loved ones has impacted their employment situation. Often, they’ve had to go in late, leave early or take time off. But 15% had to go part-time or reduce their hours; 6% had to quit working and 5% retired early.
Based on the 2019/2020 Caregiving and the Workplace: Employer Benchmarking Survey, from the Northeast Business Group of Health and AARP, employers have a way to go in recognizing the needs of their caregiving employees.
Only 9% of employers surveyed for that study said caregiving was among their Top 5 priorities for employee health and benefit issues. And although 78% of firms said their workplace culture supports employees who are caregivers, only 58% of employees said they think their top management is supportive of caregiving policies.
“There’s certainly a disconnect,” said Snelling. A Harvard Business School report on employees’ growing caregiving responsibilities, The Caring Company, backs her up. It said: “There is a gross misalignment between what companies currently provide and what [caregiving] employees need,” adding that “businesses will ignore the looming care crisis at their peril.”
Snelling, who consults with employers about caregiving, said the pandemic has led some blue-chip firms to look for ways to help their caregiving employees, especially to help them take care of themselves.
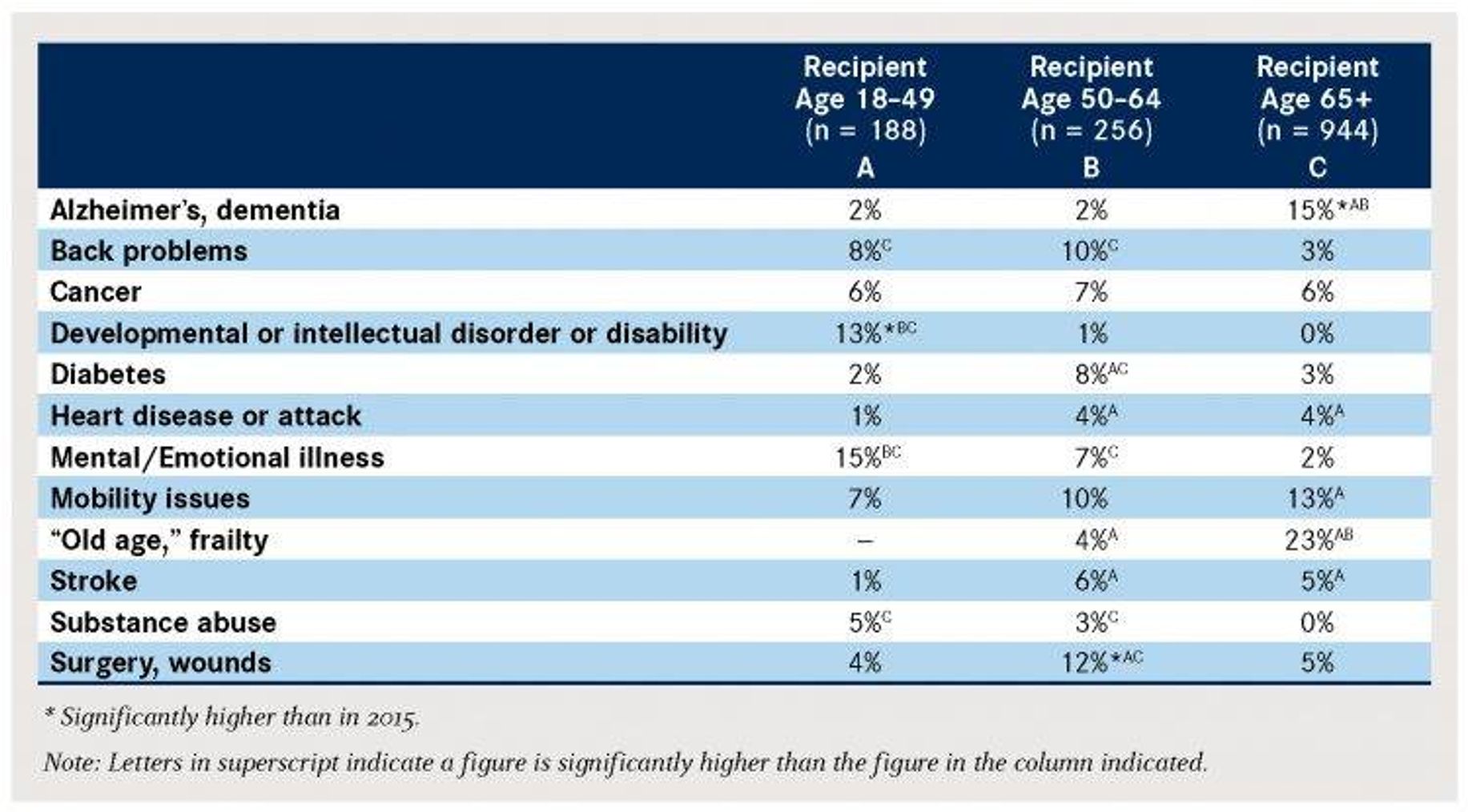
Selected Main Problems of Illness by Care Recipient
2 More Findings From the AARP/NAC Report
Two other significant findings in the AARP/NAC report:
1. Caregiving is taking a serious financial toll on many Americans, especially for those with household incomes under $50,000. An earlier AARP study found that family caregivers spent an average of $7,000 a year of their own money.
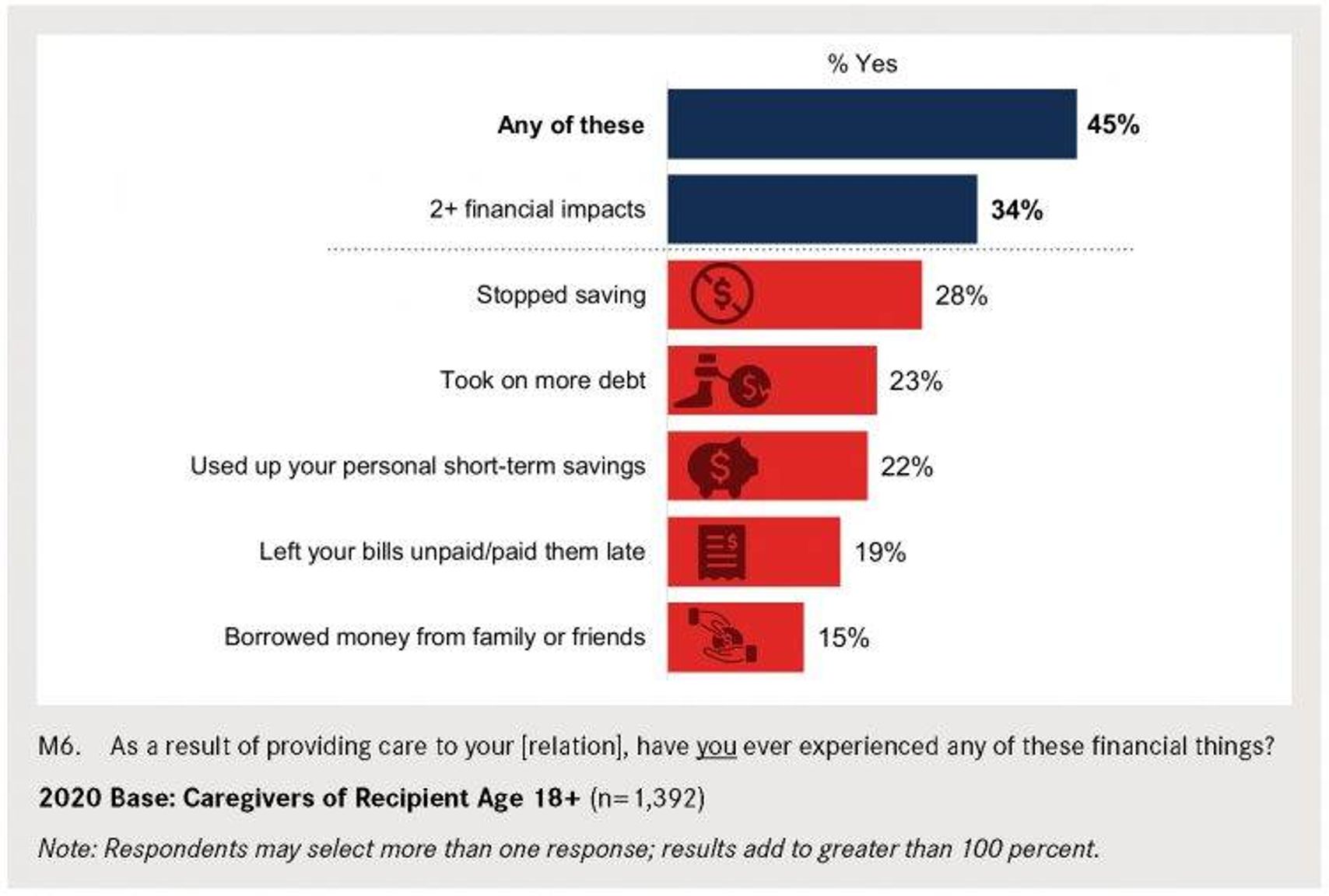
Some 45% of caregivers in the new AARP/NAC report said they’ve experienced at least one financial impact and, in what Feinberg calls “one of the more startling findings,” one in five reported a high financial strain due to caregiving.
Among the impacts: some have stopped saving, taken on more debt, used up their short-term savings, left bills unpaid or borrowed money from family or friends.
Another recent report, Still Shortchanged: An Update on Women’s Retirement Preparedness, from the National Institute on Retirement Security, said “caregiving has a highly detrimental impact on women ‘s retirement preparedness, especially if the woman is providing care for an ailing spouse.” The median wealth of women caregivers is $117,353, but it’s $276,519 for women who haven’t been or aren’t caregivers, according to this study.
2. Caregiving is particularly time consuming and intense for African American and Hispanic family caregivers. For example, African Americans surveyed said they spend 31 hours a week as family caregivers, compared to 21 hours for white caregivers.
The Families First Coronavirus Response Act offered emergency paid leave but didn’t cover medical leave for workers caring for family members with coronavirus.
Black and Hispanic caregivers are also more likely than white caregivers to assist someone needing help with at least one of the activities of daily living.
How Family Caregivers Could Be Helped
What could help America’s family caregivers?
A majority of those surveyed by AARP and NAC said these policies or programs would be helpful: an income tax credit for caregivers to help offset the cost of care; a program where caregivers could be paid for at least some of the hours they provide care and a partially paid leave of absence from work for caregivers who are employed.
In a recent MetLife employee benefit trends survey, 67% of employees said they were interested in family/caregiver leave.
The Center on Budget and Policy Priorities notes that the Families First Coronavirus Response Act offered emergency paid leave but didn’t cover medical leave for workers caring for family members with coronavirus. The think tank is calling on legislators and the Trump administration to expand paid leave to include them.
More support — from other caregivers and from employers — would be useful, too. Some caregivers don’t realize there are excellent caregiver support groups on Facebook and online. Home Instead’s free Caregiverstress.com site and HelpforAlzheimerfamilies.com site have useful advice from experts.
“I always tell caregivers: it’s OK not to be perfect,” said Goyer. “Success is not about preventing every [loved one’s] fall. There are certain things beyond our control. Success is being there.”
“This is an issue affecting all of us and our country,” said Feinberg. “We need to work together to build a more caring society.”


