What You (and Your Doctor) Don’t Understand About Dementia Might Hurt You
A new dementia survey finds stigma and misperceptions all around
Does your doctor have less faith than you in how you'd handle a diagnosis of dementia? It's possible — and that could have implications for your care.

New research suggests that misperceptions and stigma about Alzheimer's and other forms of dementia may be preventing adults from getting the help they need at two critical junctures that can alter the course of the condition: taking preventative steps and getting an early diagnosis.
According to a new AARP survey, a higher proportion of health care providers (7 in 10) perceive that patients would feel ashamed or embarrassed to have dementia than do patients themselves (1 in 5).
Doctors tend to see the sickest of the sick, a bias that can skew their perceptions of dementia and feed stigmas.
That's a 50-point difference in the data, notes Sarah Lenz Lock, AARP senior vice president for policy and director of the Global Center for Brain Health.
Doctors who are "afraid of what patients think," she adds, may be less inclined to screen for cognitive impairment and deliver a diagnosis.
"Health care providers know the end outcome and are not really focusing on the positives," Lock says. "But if you think of dementia as a chronic disease instead of as a life sentence, you have a very different view. Older adults get that — they're seeing more people living with it and understand how to adapt and be resilient."
"Folks can live for twenty years and manage Alzheimer's like a chronic disease," Lock says.
One distinction: Patients surveyed were answering hypothetically, while health providers deal with actual dementia patients. Stigma is known to cause people not to seek help for dementia symptoms, other research has found.
Doctors tend to see the sickest of the sick, a bias that can skew their perceptions of dementia and feed stigmas, said Dr. Malaz Boustani, a panelist at the Milken Institute Future of Health Summit and chief innovation and implementation officer for the Indiana University Center for Health Innovation and Implementation Science.
Other reasons contributing to misperceptions about dementia: The health care system in the U.S. operates mainly "below the neck" with little focus on cognition and brain conditions like depression and anxiety, added Boustani, who also serves on the Global Council for Brain Health.
"And ironically, there's no demand [from the public] forcing providers to do more above the neck, even though we can transplant every organ in the body — except the brain," he said.
Missed Opportunities
Presented at the Milken Institute Future of Health Summit, AARP's "2021 Survey on the Perceptions Related to a Dementia Diagnosis," offers other surprises as well.
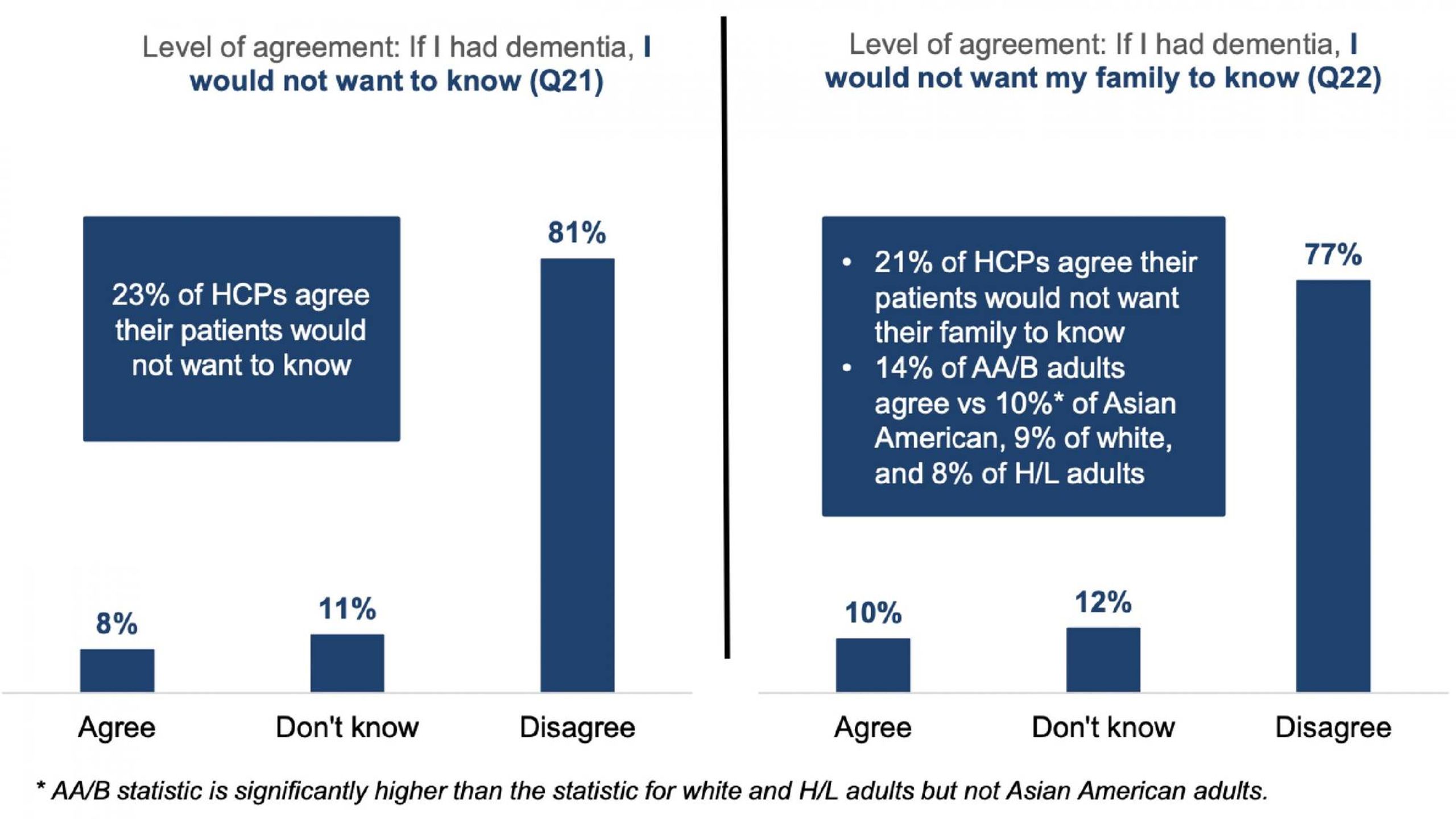
While 9 out of 10 patients want to be told of a dementia diagnosis, only 78% of health care providers said they always tell patients the truth. Providers are also more likely to believe patients would want to keep a diagnosis a secret from their families than is actually the case.
About half of adults over 40 surveyed believe it's likely they'll get dementia. In reality, only 12% will.
Stigma is one of the biggest fears around Alzheimer's, AARP research shows: fear of loss of independence (especially driving), emotional and financial suffering and fear of social isolation.
Boustani calls these the "3 D's:" driver's license, dependency and dignity.
Doctors and patients alike internalize the still-rampant stigma around Alzheimer's, says clinical psychologist Shana Stites, who was not involved in the survey. "And how people think they will react is influenced by stigmatizing beliefs they may hold," she says.
Stites studies Alzheimer's stigma and is a faculty investigator with Penn Memory Center's Penn Program on Precision Medicine for the Brain.
She notes that health care providers still fall into two camps: those who follow up and directly address stigma with patients and those who feel it's best not to disclose anything for fear of harming their patients' quality of life and because they want to protect patients against bad outcomes.
Doctors who have internalized stigmas around dementia, Stites adds, may note the dearth of disease-modifying therapies and avoid offering cognitive tests in the first place.
"They miss that patients often say, 'Had I known earlier, I'd have done things differently,'" she says, in terms of how they spend their days, prepare their estates or engage in preventative care.
Early diagnosis is also the gateway to clinical trials and early-intervention therapies like the new Alzheimer's drug aducanumab, marketed as Aduhelm.
When doctors address stigma head-on with patients, Stites' research shows, patients wind up feeling more empowered and less likely to have self-fulfilling negative expectations.
Missed Prevention Opportunities
Another jarring discord unearthed in the AARP survey was between patients' perceptions of getting dementia and what they're willing to do about it.
About half of adults over 40 surveyed believe it's likely they'll get dementia. In reality, only 12% will, Lock says. The survey result declines slightly with advancing age, with those 40 to 49 being most pessimistic about losing cognitive function.
Yet a slight majority of respondents say they don't want, or don't know if they want, a yearly cognitive exam. And while 67% were open to an annual cancer exam, just 46% would like the same for dementia. (About half would like a baseline cognitive evaluation.)
What's more, other research from AARP and elsewhere has shown that adults are slow to adopt brain-healthy behaviors that have been found to alter the trajectory of cognitive decline, like improving nutrition, exercise and sleep.
"Behavior change is hard," Lock says.
In July, AARP is kicking off a series of events to address the gap between what science now knows works, preventatively, and what people actually do. (In a related outreach effort, through the end of June 2021, its Staying Sharp Brain Health Assessment is free to AARP members.)
Three-quarters of health care providers surveyed agree that adopting brain-healthy behaviors can help. Just 4 in 10 adults are aware there is no cure for dementia, the survey found.
The AARP report was based on a survey of more than 3,000 adults ages 40 and older, as well as a survey of providers in family and internal medicine, geriatrics, neurology and psychiatry/psychology.

Read More

