Kidney Dialysis: Prolonging Life or Prolonging Death?
A doctor's father considers whether the procedure is worth the risks and difficulties
(This article was provided by The OpEd Project.)
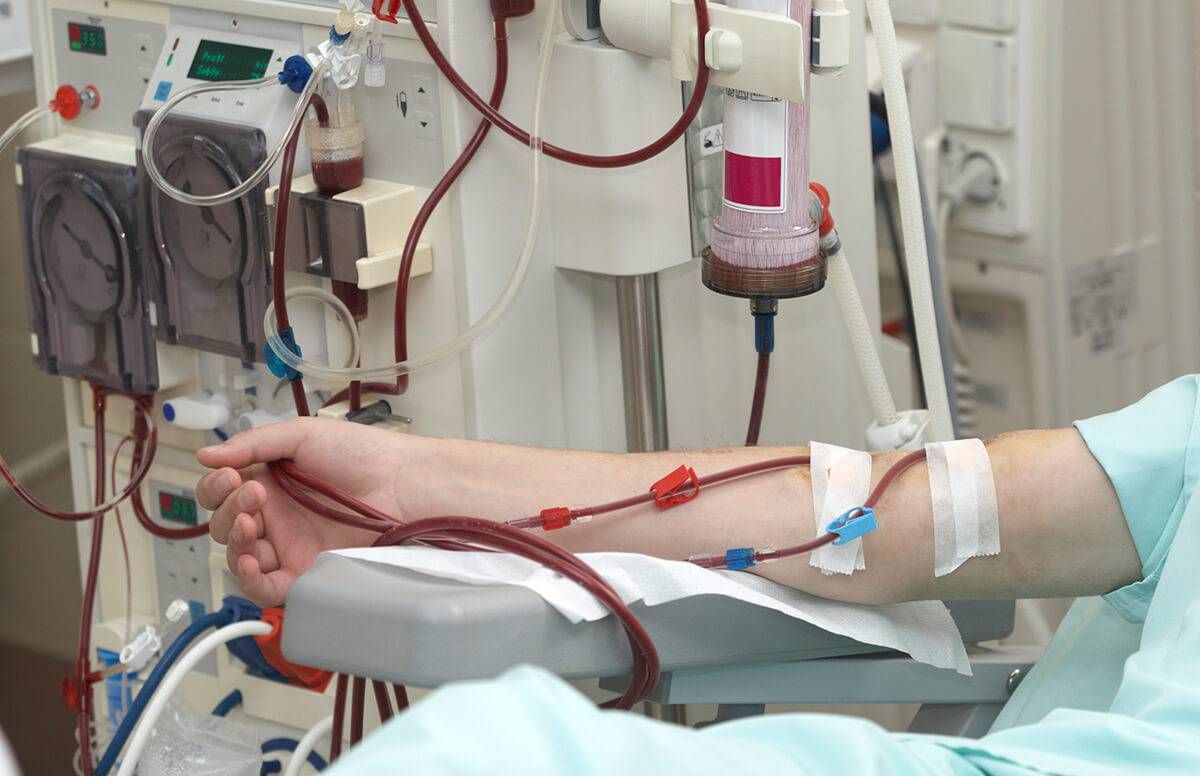
My father was dying. Thirty years of diabetes had destroyed his kidneys, nerves, blood vessels and eyes. He had anorexia, nausea and lethargy. His skin was streaked with angry itch marks. Proteins were draining out in his urine. Calcium was leaching from his bones. His toes were cold and blue and painless, without sensations. His deteriorating balance made even walking unsafe. He slept after every meal, the effort exhausting him.
Dad was 82 years old and had end-stage renal disease.
One in seven Americans has some form of chronic kidney disease. According to the National Kidney Foundation, about 30 percent of patients with Type 1 diabetes and 10 to 40 percent of those with Type 2 diabetes eventually will suffer from kidney failure.
The majority of those with chronic kidney disease won’t know it because the disease is asymptomatic in early stages. But some will progress to end-stage and will need renal replacement therapy, dialysis or a transplant to live.
Medicare spending for patients with chronic kidney disease exceeds $50 billion, representing 20 percent of Medicare spending, with an additional $31 billion spent on the more than 660,000 patients with end-stage renal disease.
Kidney Dialysis: ‘His Only Option’
Dad was too frail for a transplant. Dialysis was his only option, his doctor said.
Without doubt, dialysis extends life and is critical for patients waiting for a kidney transplant that may take several years. Patients who have no, or few, other diseases could get dialysis in a clinic or at home and go about their day as usual. My father needed dialysis three times a week, four hours each time. He would be tethered to a dialyzer for several hours for the remainder of his life.
Would dialysis prolong life or prolong dying? My father was confused.
Making the Case for Dialysis — Or Not
Dad was an engineer. He preferred data. As a professor at the Yale School of Medicine, I could analyze and summarize the medical literature for him, succinctly. I felt that I could help him make the most important decision of his life.
But studies on dialysis in octogenarians are scant, and the benefits controversial.
According to Dr. Manjula Kurella Tamura of the Stanford University School of Medicine, the majority of nursing home residents on dialysis suffered a substantial and sustained decline in functional status after its initiation. Dialysis could not guarantee improvements in symptoms or depression.
The New England Journal of Medicine reported that six months after starting dialysis, one in three octogenarians had died and only 28 percentremained independent. In Canada, 60 percent of the elderly on hemodialysis (a type of renal replacement therapy) regretted their decision after six months as the symptoms persisted or worsened. The burden of symptoms in older adults on dialysis rivaled that of cancer. One in three octogenarians ultimately discontinued dialysis, rejecting an unacceptable quality of life.
Costs Significant
Older people generally have multiple chronic conditions and are prone to infections and other complications requiring additional hospitalization. The annual cost of hemodialysis in people older than 67 is significant: $115,000 per person. With each extra day my father lived, the risk of gangrene, blindness, falls and fractures increased, and the survival time gained might be spent in the hospital.
Dad likened going for dialysis thrice weekly to going back to work, “without pay, like volunteering.”
If they chose that option, my mother would go with him despite her crippling arthritis. For her, too, it would also be like going to work, at 75 years of age. My sister would drive them. They would all spend less time with my sister’s little girl, the light of their life.
Home dialysis was considered. My mother would need to learn to connect him to bags of dialysate (a fluid used in dialysis) through a permanently-placed tube in his abdomen.
“Wouldn’t that cause infections? With the dogs around?” Dad wondered. It could. They had two Pekingese.
Unanswered Questions
“My doctor didn’t explain it to me,” Dad said, frustrated. “Not like this. He said dialysis was the only option since I am too frail for a transplant. He said I could even live for 20 years. I don’t want to live like this!”
Dad made his decision — no dialysis — the option his doctor hadn’t mentioned.
Shared decision making requires taking into consideration the patient’s quality of life, his wishes and goals and sometimes, helping him choose one option over the other. It requires of the physician good nonjudgmental listening and complete honesty. Violating the dignity of an incurable patient, using science to stop the inexorable march towards death, interfering with a “necessary end” should not be acceptable in any society, however advanced or civilized.
My father died seven months later, at home amidst his loved ones who had bravely struggled to let him live, or die, as he wished.

