You Need a Ventilator. But Do You Want One?
Get to know the device, how it's being used and its risks
Editor’s note: It's been quite a year. Through it all, we haven't stopped reporting on what matters to older Americans. In these final days of 2020, we're featuring a selection of our most read stories, including this one. Through a coronavirus question submission form, our readers inquired about how and when ventilators are used in COVID-19 — and how to decide whether to go onto a ventilator for life support if offered. This, and more, is addressed in the below story.
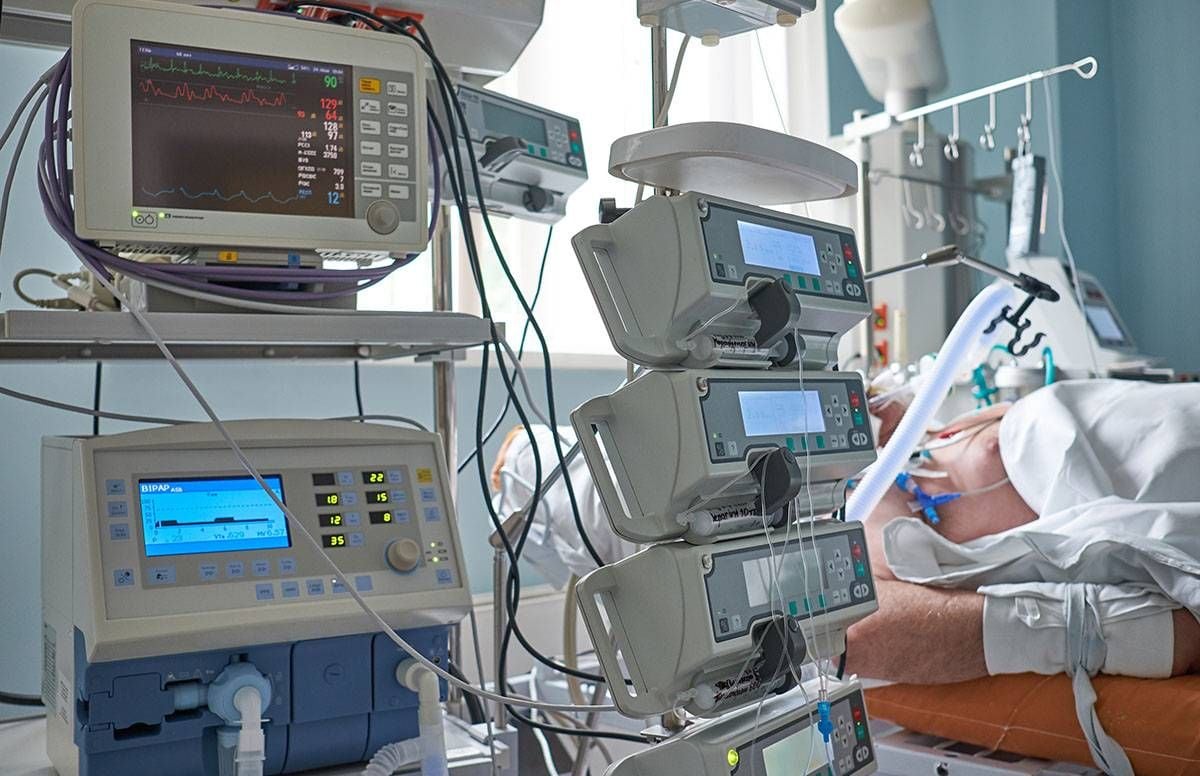
Ventilators have possibly never been as central to public discourse as they have been during the COVID-19 pandemic.
First it was the grave shortage of the device in Italy, where doctors were left to make excruciating choices about which patients would receive breathing help from a life-sustaining mechanical ventilator. Since the virus' outbreak in the U.S., the conversation has evolved into the safety of the ventilator and the medical community debating the appropriate circumstances to hook a patient up to one.
Ventilators are now only being turned to as a final measure to save a patient's life.
Health care providers express concern that prospective patients and anxious Americans aren't equipped with a baseline understanding of what it means to go on and then come off a mechanical ventilator, how the machines are being deployed in U.S. hospitals and — most importantly — the necessity of using this information to decide what you would want should you become seriously ill with COVID-19 and the device is offered.
When Are Ventilators Used for COVID-19?
Though doctors were quicker to trigger the use of ventilators early on in COVID-19's appearance in U.S. hospitals, the thinking is now more on the conservative side.
"Initially we thought we'd see patients get rapidly worse, and we would rather place them on a ventilator in a more controlled fashion than in a crisis where they're crashing," explains Dr. Marc Rovner, a pulmonologist at Indiana University Health's Methodist Hospital in Indianapolis, who, as of late April, has provided care to around a dozen COVID-19 patients.
Rovner says health care providers are backing away from intubating patients (part of the ventilator process where a tube is inserted into the windpipe) as early as before. Now, doctors are first leaning on other methods of breathing assistance, like the use of high-flow oxygen — a non-invasive form of ventilator.
What's fundamental in understanding the purpose of ventilators for COVID-19 is that they're currently only being turned to as a final measure to save a patient's life when without one, a person is likely not to survive the disease.
Our Commitment to Covering the Coronavirus
We are committed to reliable reporting on the risks of the coronavirus and steps you can take to benefit you, your loved ones and others in your community. Read Next Avenue's Coronavirus Coverage.
"We don't go right from being OK to being on a ventilator," says Rovner. "We try to wait as long as possible and look for trends that [patients are] getting better. We put you on a ventilator because we think it's [the coronavirus] getting worse: more shortness of breath, breathing faster, getting very anxious about breathing, oxygen saturation below a point in which we consider safe."
Doctors must weigh whether a ventilator's complications (more on that to come) are worth using the ventilator to give the patient enough time to recover from COVID-19, which can take weeks on the machine.
While patients over 80 have a low survival rate on a ventilator, Rovner says someone who is otherwise mostly healthy with rapidly progressing COVID-19 in their 50s, 60s or 70s would be recommended a ventilator to let their lungs heal.
Dr. David Hill, a pulmonary and critical care physician at Waterbury Hospital in Waterbury, Conn. and board member of the American Lung Association, has frequently been making judgment calls on the right time to place COVID-19 patients on ventilators.
"Sometimes it's obvious when you're looking at a patient. But there's other patients where they're sick and working hard to breathe and you have to make that decision of: Is this the time to do this or not?" he says. "There's also a window of opportunity where if you wait too long, they don't do as well because their disease is more advanced when you put them on the ventilator."
What It's Like to Be on a Ventilator With COVID-19
Here's a rundown of what being on a ventilator with the coronavirus is like:
It's not comfortable. Mechanical ventilators are a form of life support. Because of the invasive nature of hooking someone up to a breathing machine, patients must be heavily sedated to relax and tolerate the discomfort.
You won't be able to communicate. On a ventilator, you can't talk and you won't be aware of your surroundings.
You may be on one for a long time. When a COVID-19 patient requires mechanical ventilation support, it's not just for a couple days. Two to three weeks is not an unusual time for patients to be on ventilators — sometimes longer. Beyond that, patients may require a procedure called a tracheostomy, where a tube is inserted in the opening of one's neck rather than down the windpipe.
There are complications. Among them, the pressure from a ventilator can make a patient's lungs collapse or increase the risk for pneumonia. As much as a quarter of patients intubated with COVID-19 experience their kidneys shutting down. Over time, doctors use lower volumes of oxygen with lower pressure to cause less injury, but ventilators are still "not completely safe and harm free," says Hill.
It's difficult to come off a ventilator. Doing so takes a long process called weaning, where patients gradually begin breathing on their own. Some patients will struggle with coming off mechanical ventilation and some will then need to be put back on.
Afterward, you'll need rehabilitation. This usually involves physical and occupational therapy to get up and moving again. Eventually, a patient will transition either home or to a rehabilitation facility. The recovery period will be longer for an older person who has other medical conditions.
Mental health may suffer. A quarter of patients will have post-traumatic stress disorder (PTSD) related to having a near-death experience. They'll require counseling and medications. A large percentage may not return to their fully-functioning lives.
Life can significantly change. Looking at the outcomes of acute respiratory distress syndrome (ARDS), which has similarities in treatment to COVID-19, Hill suggests about half of COVID-19 survivors, like ARDS survivors, may not be able to return to work full time. And a quarter may not be able to return to work at all. "But we really don't know what to expect," he says. "Six months ago, there was no COVID-19, so we don't know what the long-term effects are because we need time to see what the underlying, subtle effects of this disease are in the people who had it and survived."
How to Decide If You Want a Ventilator
In nearly all COVID-19 cases, the choice between using a mechanical ventilator or not is the choice between life and death.
So, the question becomes, knowing the process, the risk factors, your quality of life and health: If you were to fall extremely ill to COVID-19, would you want to do everything possible to stay alive if it meant going on life support including a mechanical ventilator?
"It becomes a very personal decision," says Hill. "If I'm seeing somebody in their mid-eighties who had health conditions that put them at risk, we're more likely to stress the fact that they're unlikely to survive if they go on a ventilator, as opposed to seeing somebody in their fifties who might just have diabetes or high blood pressure."
At Cleveland Clinic hospitals, several COVID-19 patients have turned down ventilators once they understood that what was involved was not consistent with what they wanted, says Dr. Hassan Khouli, chair of Cleveland Clinic's department of critical care medicine. Patients always have the option to be made comfortable for the end of life rather than fight to survive, if their chances are unlikely.
"There is enough suffering going on, and we don't need to add to it by not knowing what people wanted."
Dr. Kathryn Dreger, an internal medicine doctor in Arlington, Va., recently outlined what patients should know about ventilators in an opinion piece for The New York Times. Dreger sees her patients in all settings, including the ICU, where she recently cared for a patient who fell ill with COVID-19.
"A lot of people are going to die on the vent, which is a lousy way to die," she said in an interview. "A lot of family are going to have to say, 'What did mom or dad, husband or wife want me to do?' And have to make it up because they're not able to be there by their side or not able to ask."
Dreger underscores the necessity of, at the very least, communicating to family members, trusted friends or a health proxy (someone legally appointed to make health care decisions on your behalf when you cannot) your basic wishes regarding the use of invasive life support.
Additional questions to consider, which Dreger describes as a "very depressing menu at a restaurant," include:
- What’s the longest you would want to be hooked up to a mechanical ventilator?
- If you required a feeding tube through a hole in your throat or stomach, would you want to continue on the ventilator?
- Are you up for a prolonged rehabilitation that may involve going to a nursing home?
"You can say, 'I'm going all the way. I'm going to crawl over the finish line covered in blood if that's what it takes,'" Dreger says. "But there is enough suffering going on, and we don't need to add to it by not knowing what people wanted."


