Genetic Testing and Counseling for Breast Cancer Can Help Guide Decisions
But every woman can and should make her own choice about treatment
(Editor’s Note: This article is part of a collaborative reporting series between the American Cancer Society and Next Avenue. The series is exploring the state of genetic testing in breast cancer patients.)
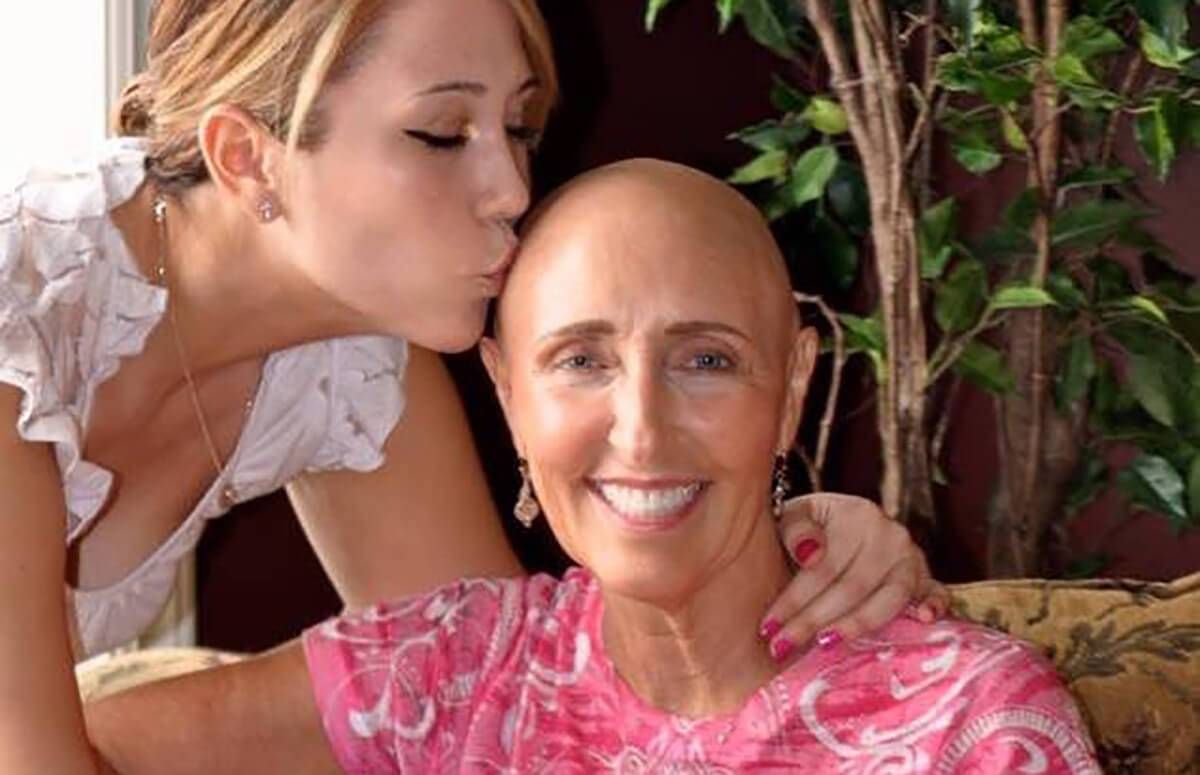
After a routine mammogram in 2014 revealed a tumor in her right breast, Wendy Mayer was diagnosed with invasive lobular carcinoma. Fortunately, it had not spread. But her mother, her grandmother and a cousin had all had breast cancer, so on the advice of her doctors, Mayer underwent genetic testing.
“I think waiting for those results may have been the most stressful part of this entire thing,” the Washington, D.C.-area resident said. To her great relief, it showed she did not have a harmful mutation on either the BRCA1 or BRCA2 genes. (Mutations in these genes are linked to an increased risk for breast and ovarian cancers.)
That knowledge made Mayer, now 67, comfortable with her treatment decision. She had a lumpectomy, which allowed her to keep most of her breast. The alternative was what she said she would have probably chosen if she did have a mutation: bilateral mastectomy, the removal of both breasts.
Getting Answers About Breast Cancer
Women newly diagnosed with breast cancer face so many unknowns: What does the diagnosis mean for my future? What kind of treatment is best? Did I inherit a high-risk gene? What effect will my cancer, if it is genetic, have on my children or grandchildren?
Genetic testing can answer some of those questions. But what precedes and follows that test is vital, experts say. Many women have been helped by genetic counseling, a detailed discussion by a trained professional of a woman’s specific circumstances.
“Genetic testing is very complicated; it’s not a simple blood test,” said Suzanne Mahon, a registered nurse and genetic counselor at Deaconess Cancer Center in St. Louis. “The interpretation … hinges not only on the test results, but also on the personal and family history.”
Unfortunately, not everyone has equal access to such counseling. And research has shown that many women fail to get it because their doctor didn’t suggest it, as noted in the first story of our collaborative reporting series with the American Cancer Society. Instead, most newly diagnosed women first see a surgeon.
Kathy Bressler is thankful that she had the benefit of counseling after her breast cancer diagnosis.
“That was such a positive experience,” said the 56-year-old Omaha hospital administrator. “I felt really comfortable that we had done the latest testing and that it showed everything that there was to show at the time.”
Genetic tests are far different now than they used to be. Previous tests looked for mutations on only the BRCA genes, but today’s genetic tests can identify variations associated with breast cancer on 20 or more genes. The tests are also far less expensive now.
A Family History
Like Mayer, Bressler also had a mother with breast cancer. But Bressler was relieved to learn through a genetic test about 15 years ago that she did not have any harmful BRCA mutations. Nevertheless, a sharp pain in her right breast in December 2015 led her doctor to recommend an ultrasound. It revealed a 1.7 cm lump.
A new genetic test showed no harmful mutations on any of the genes, but the breast biopsy revealed a darker result: She was diagnosed with triple-negative breast cancer, in which the three most common proteins involved in tumor growth are missing, thus ruling out several treatment options. It's “the kind you don’t want to have,” she said.
Though her medical team encouraged her to choose a lumpectomy, also known as breast-conserving surgery, Bressler didn’t hesitate: she wanted a bilateral mastectomy. “I was 27 when my mom died, and I just knew I wasn't going to mess around,” she said. “I wasn't going to have mammograms every six months and worry and stress.”
A subsequent test made her even more convinced that her choice was a good one: An examination of the breast tissue after mastectomy revealed three additional tumors.
Bressler said she always encourages other women to get genetic counseling and testing if they have any family history of breast cancer. “I think it really helps women in their decision-making. Without that information before surgery, you're not making a completely informed decision,” she said.
She also emphasizes early diagnosis through regular mammograms and other screening as appropriate. Bressler urges women to be aware of their own breasts and report any changes to their doctor. And she encourages everyone to help fund breast cancer research.
“That's where we learn about more of the genes that are indeed connected to breast cancer, and that's really important,” she said. “We're not done learning about what causes breast cancer.”
Choosing Your Own Path
Christine Thies, 48, of Austin, Texas, also chose a double mastectomy — even though genetic testing revealed no harmful mutations. Her mother had died of breast cancer and Thies was diagnosed with it after a breast reduction surgery, when her tissue was tested.
“I’m not good with the unknown,” she said. “I tend to be pretty analytical, and for me, it was a numbers game.”
But she would never describe her decision as something that’s best for others.
“Everyone has their own journey, and everyone comes to this decision differently,” she said. “There is no right answer. You just have to make an answer that is best for you.”


