7 Ways to Make the Most of Your Hospital Stay
With the American Hospital Association reporting more than 33 million people were hospitalized last year, chances are you or a loved one will need an inpatient hospital stay
I spent five days in February with double pneumonia at our local hospital. Retired from three-plus decades in a health career, I know a hospital is often chaotic. And I also recognized that change still rules. Nevertheless, I knew what to expect. As a patient or a loved one's advocate, knowing what to expect may diminish anxiety and assist in healing.
Prospective Payment for Medicare and Medicaid (a significant change) began months after I started my first hospital job. If Grandma had nobody at home after hip surgery, her doctor could keep her in the hospital, sometimes for weeks.
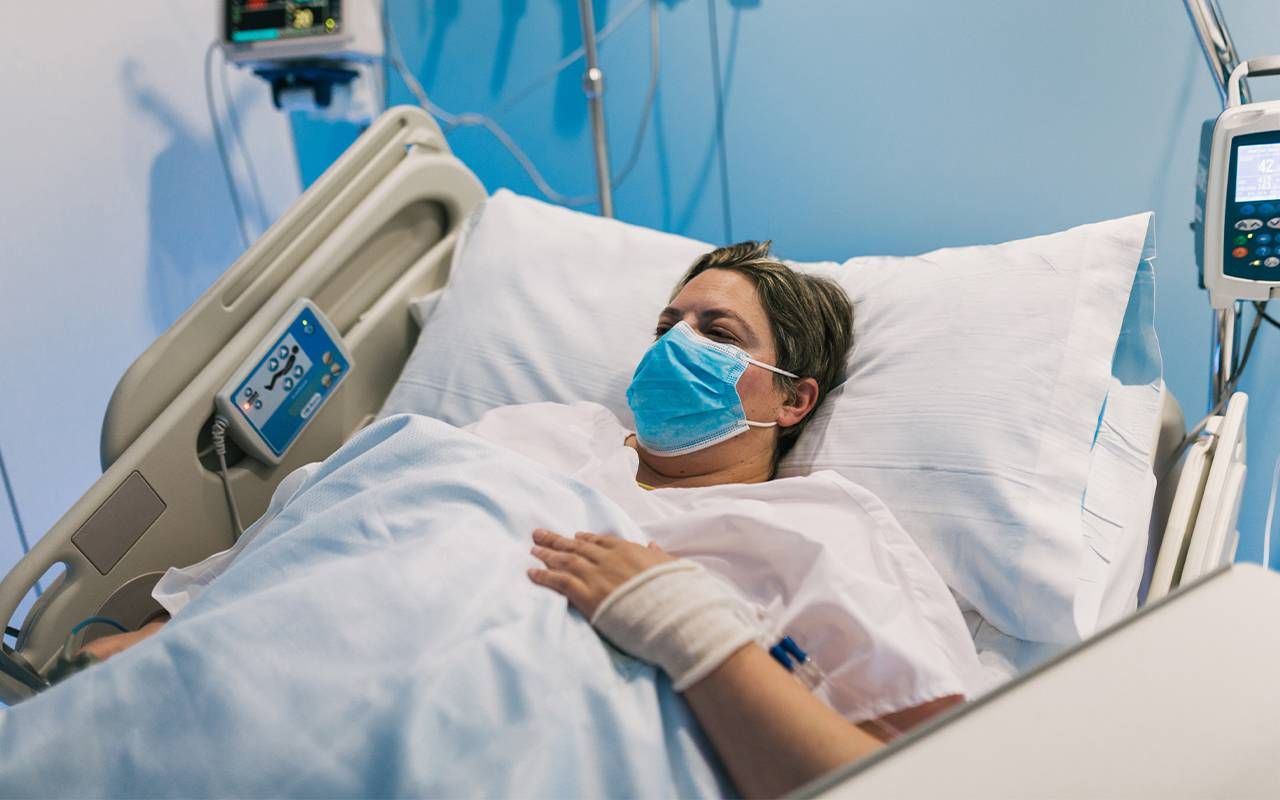
Hospital staff and patients alike share the desire for improved health for patients, but things don't always go according to plan.
Thus, the new payment method encouraged shorter hospital stays and the boom of outpatient care, free-standing surgery centers, home health care agencies, stand-alone specialty hospitals and hospital-owned physician practices to maximize hospital revenue.
But, unfortunately, COVID slammed into us like a hurricane.
As a result, our health care system experienced short staffing, supply chain issues and the move to telehealth. But at the core of health care is care. Hospital staff and patients alike share the desire for improved health for patients, but things don't always go according to plan.
7 Ways to Advocate for Yourself or a Loved One
Regardless of your situation, you can be your best advocate or have a family member serve in that role if you are unable. Here are seven considerations for being the best advocate for yourself or a loved one during a hospital stay:
These items may spark a conversation that will avoid more anxiety during the hospital stay.
- Bring what you need. As simple as this sounds, you will need essential items not provided by the hospital. I keep a travel list on my computer, and I wish I had kept a hospital list. I didn’t realize my Emergency Department (ED) visit would turn into five days in inpatient care. Round up your bathrobe, slippers, extra glasses, phone, phone charger and whatever is needed away from home. Pack a small notebook and pen, or find the notes app on your phone. Bring a copy of your advanced directive. You may be admitted into a 23-hour observation bed. Accepting patients to a specialized ED area is now considered best practice so patients can be observed in a clinical setting (depending on your health, you may be sent home or upstairs at the end of 23 hours).
- Your doctor may not see you during the hospital stay. Physician staffing is handled by hospitalists, who are hospital employees, and work long shifts. Call or have your advocate contact your personal physician’s office and let them know you are hospitalized. For example, an RN friend suggested I call my primary doctor after my Saturday admission, and the office called me Monday morning at the hospital. The call triggered the office to check my electronic medical records for updates.
Call or have your advocate contact your personal physician's office and let them know you are hospitalized.
- Learn about hospitalists. Your in-house provider may have rounds late in the morning, as physicians once did. Hospitalists are there all day. Be prepared for your provider to visit anytime, and write down what you learn in your notebook or phone app. The rotation of a hospitalist may vary from weekends to seven days on and seven days off. Notes help you or your advocate recall information from another provider.
- Are you what the pros call a “hard stick?” Let your primary nurse know you want someone from the phlebotomy department for your inevitable blood draw. I am a hard stick and would rather have needles in my eyes than venipuncture (having had injections in and around the eyes, I know how it feels). My usual protocol is for the person drawing my blood to put a butterfly clamp in my hand and slowly and painfully remove five tubes of blood. During my recent hospital stay, I immediately told my nurse about my concern; two Super Phlebotomists arrived. My heroes brought a machine that could identify the best vein for venipuncture. The draw was painless.
- Ensure everyone who visits your room knows who you are and what is essential to know about you. Write on the whiteboard, if necessary: “Amy, difficult blood draw.” During your stay, you may encounter case managers, therapists, admissions personnel, lab workers and direct care staff. Hospitals today are like siloes; because so many people work with patients, information can be misconstrued or absent. For example, my digestive care doctor sent me to a hospital for a routine colonoscopy because I use supplemental oxygen. I assumed the hospital staff knew of my need. In recovery, my worried husband asked the nurse about my oxygen. Not only was the recovery room staff unaware that I used supplemental oxygen, but it had also been taken off after my procedure in the surgical suite. My portable compressor was with my clothing underneath the gurney. Now, at any procedure, I make sure everyone knows I wear oxygen and why.
- If you aren’t ready for discharge, express your opinion, and tell the doctor why. Are you too unsteady on your feet? Feeling unsure of meds? Have no one to change bandages? Extending your stay may lower reimbursement for hospitals. However, there may be medical and legitimate reasons for the extension. Do you need to go to rehab or home care? Again, speak up; the physician is not a mind reader.
- Make sure you understand your discharge orders when leaving the hospital. And if you have questions at home, call. Double-check with your pharmacist for interaction on any new medication. Keep all aftercare appointments and pay special attention to your health post-hospital time. Healing is not finished when you get in the car to go home from the hospital.
These tips are common sense, but sense may fly out the window during an illness. Patients must self-advocate or have someone who can serve in that role. While pondering a future hospital stay, share this article with your advocate. Get your advance directive in order. These items may spark a conversation that will avoid more anxiety during the hospital stay. Get things in order, forget about it until the need arises, and live your best life.
Next Avenue and the author do not offer this piece as medical advice. A patient or advocate should always discuss clinical issues with a medical provider.


