5 Over-the-Counter Meds You May Be Misusing
From acetaminophen to nighttime cough and cold medicine, using them wrong can cause big problems
1 of 7

We’ve all done it — taken three aspirin instead of two for a particularly bad headache, or gulped some NyQuil to help us sleep, even if we’re not really sick.
Using over-the-counter (OTC) medicine in ways that aren’t intended may seem like no big deal at first, but harmful drug interactions and overdose can be more problematic than you think. For example, around 30,000 people are hospitalized every year for taking too much acetaminophen, according to The New York Times.
Read on to learn about five of the most commonly misused OTC drugs, how they affect your health and how you can avoid using them incorrectly.
(This article appeared previously on Grandparents.com)

1. Acetaminophen
It's estimated that about 150 Americans die each year by overdosing on acetaminophen. Generally speaking, these kinds of overdoses aren’t intentional; the drug is a common component in a variety of medications, which can make it difficult to tell how much we’ve really ingested.
"Acetaminophen can be found alone in products, in cough and cold combination products and combined in prescription pain relievers," says Maria Mantione, spokesperson for the American Pharmacists Association. "It ‘lurks’ in so many places, you can accidentally take too much."
Overdose can lead to liver problems or possibly death, so it’s important to monitor your intake. "Always carefully read the drug label on the package to determine how much acetaminophen a product contains," says Alexander Tu, an official for the National Community Pharmacists Association. "Do not take more than 3000 mg in a 24-hour period."

2. Some Heartburn Medications
More than 15 million Americans use proton pump inhibitors (PPIs), a.k.a. heartburn medications like omeprazole (Prilosec), annually. Overdose can cause problems including confusion, blurred vision and vomiting, while prolonged use may lead to inflammation of the stomach lining and depleted magnesium levels.
Even more alarming was the news from two studies earlier this year that found that PPIs may be linked to an increased risk of chronic kidney disease and dementia.
So, it’s important to take PPIs only as directed.
"PPIs should be reserved for occurrences of heartburn symptoms two or more days a week," says Tu. "Also, PPIs should only be used for no more than 14 days...every four months."
If you need instant relief, Tu suggests trying another route, "Take an antacid such as calcium carbonate (Tums) or an histamine-2 receptor antagonist (H2RA) such as ranitidine (Zantac)."
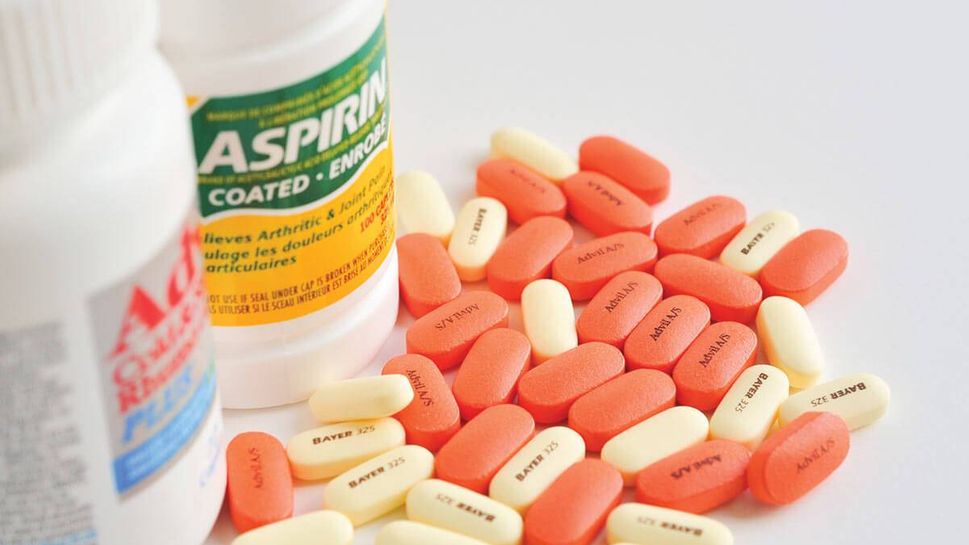
3. Aspirin
Back in the day, aspirin was used to combat pain and fever. Nowadays, it’s taken largely for heart attack and stroke prevention, frequently by older adults who need to be aware of mixing it with other meds. "Aspirin should not be combined with other anti-inflammatory pain medications, like ibuprofen and naproxen, as combining them can lead to increased risk of stomach bleeding and kidney problems," says Mantione.
If you’re considering an aspirin regimen or are already among those popping a daily pill, speak to your pharmacist about potentially harmful interactions — both with your existing prescriptions and other OTC drugs.

4. Nighttime Cough and Cold Products
"If your sole purpose is to help you sleep, you should not take a product like NyQuil because it contains more than just a sleep aid," says Mantione. "Combination cough and cold products often contain many ingredients, sometimes four or five different drugs, and although they seem convenient, you likely will be ingesting a medication you do not need, which leaves you prone to side effects and interactions that could have better been avoided."
As a general rule, you should never take drugs for illnesses you don’t have. "Taking medications that have active ingredients that treat symptoms not present can cause unwanted side effects as well as potentially interact with other medications," reinforces Tu. Instead, for that nagging short-term insomnia problem: "Supplementing with melatonin, turning off the TV while in bed or establishing regular sleep hours may help," he says.
5. Nasal Spray
Decongestant nasal sprays are among the most misused OTC drugs because they’re administered too often for too long. "If you use them for more than three days, which many people don’t know, they can lead to rebound congestion, which can cause you to need them more — and that cycle makes it hard to stop them," says Mantione.
Should you choose to use nasal spray, go easy: limit your use to a few times daily, and stop after three days. Note, too, that decongestant eye drops meant to reduce redness can have the same effect. "With overuse, they can lead to bloodshot eyes, making you reach for them again," she says.
How to Avoid Misusing OTC Drugs
To decrease the chances of an adverse reaction to OTC medications, follow these rules:
— Read the labels carefully. "Not just the front of the box, but the back, where it tells you who should avoid the medication, how much is safe to take and what interactions it can cause," says Manzione, who tells her patients to keep a magnifying glass close by for smaller print.
— Be especially careful administering them to children and the elderly. "These populations tend to be more vulnerable to the effects of medications," says Mantione. What’s more, kids’ doses are often different and older adults can have multiple prescriptions, increasing the chances of harmful interactions.
— Just ask or pharmacist or physician. Says Tu: "The best strategy to avoid the misuse of OTC drugs is to ask your pharmacist or doctor whether a particular OTC drug is right for you." Make sure you tell them about everything you’re taking, from medications to vitamins.
Grandparents.com is a lifestyle website, social media community & peer group that unites & connects America's 70 million Grandparents to the best information and premier products & services just for them. Our goal is to promote well-being and give timely information on what really matters to you, from health and money to family and relationships to travel and retirement.

