When Wounds Won't Heal
What works for wounds that haven't closed within 30 days
You've developed a huge blister from dancing in three-inch heels or gotten a nasty gash in your hand while sawing through wood, injuries that normally heal easily. But if you have diabetes, venous insufficiency (improper functioning of vein valves in the leg) or other medical conditions, you may be one of the unlucky people who develops what's called a non-healing or chronic wound.
These are wounds that have failed to progress through an orderly sequence of repair in a timely fashion and which haven't closed within 30 days. Then what? (Warning: some icky stuff follows.)
"The procedure was totally painless, the nurses and other staff were wonderful and the wound healed very well."
Chronic non-healing wounds affect approximately 6.5 million people in the U.S. and more commonly occur in older people, many of whom have comorbidities such as diabetes, vascular disease, chronic venous insufficiency and obesity.
Other conditions that hinder wound healing include being immunocompromised, certain types of cancer, peripheral artery disease or connective tissue diseases such as rheumatoid arthritis, taking medications like steroids or chemotherapy drugs, and smoking.
Going Into 'Dives' for a Wound
Nancy Michelian, 61, a nurse in Harrisburg, Pa., knows all about non-healing wounds. She was diagnosed with breast cancer in 2010 and treated with a lumpectomy and radiation therapy. For a 2017 recurrence, she had a mastectomy and underwent chemotherapy. After surgery, she went home with a drain in her chest. Drainage from the wound was expected to stop within a week, but pockets of fluid continued to seep out way beyond that.
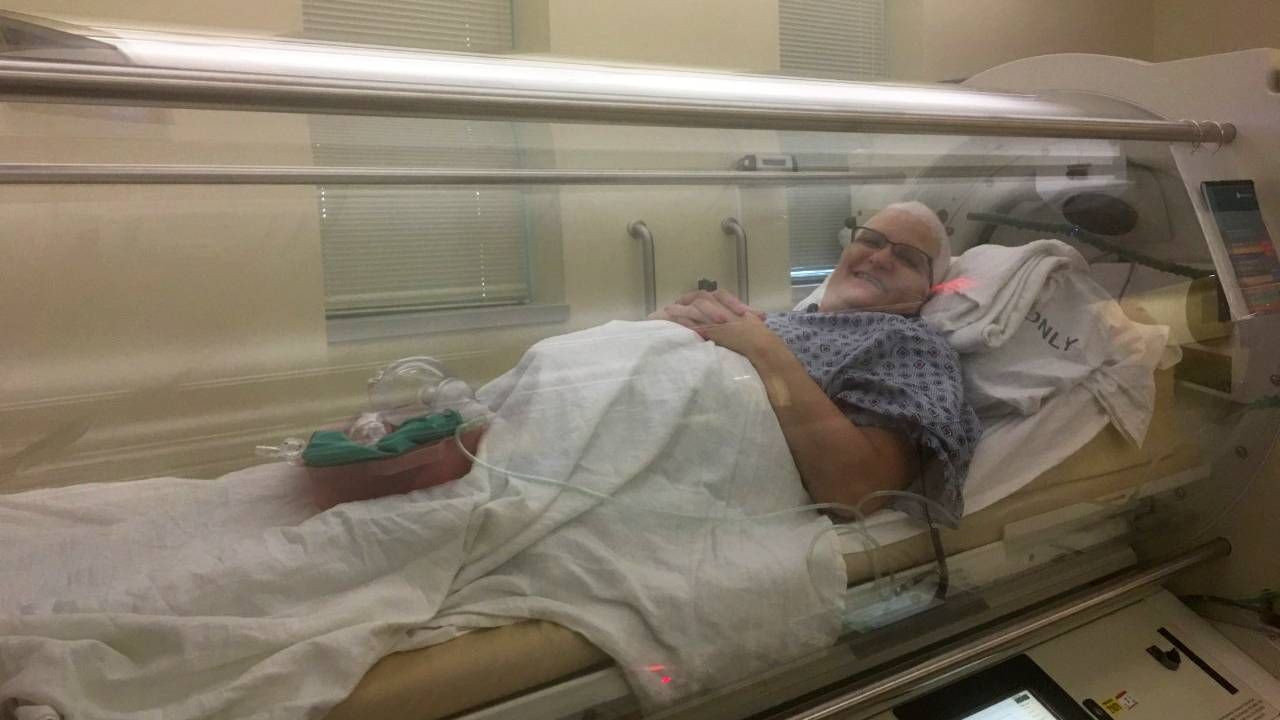
The deep wound, 4 inches across and 1 ½ inches wide, didn't heal well because the skin had been damaged by the radiation treatments. Along with other therapies, she had 24 sessions in a hyperbaric chamber at the University of Pittsburgh Medical Center Pinnacle Wound and Hyperbaric Center in Harrisburg, Pa. They're referred to as "dives," and each lasted around two hours.
"The procedure was totally painless, the nurses and other staff were wonderful and the wound healed very well," says Michelian.
The most common chronic wounds are vascular (arterial and venous) ulcers and diabetic foot ulcers. Pressure ulcers — also known as bedsores — occur when there's a prolonged period of immobility which leads to skin breakdown and ulceration, especially on the back, ankles, feet and buttocks.
Understanding Wound Healing
Wounds can heal in different ways. Primary intention wound healing occurs when wounds are closed using stitches, staples, butterfly strips or other closures. Secondary wound healing occurs when — due to location, shape of the injury or other factors — a wound can't be satisfactorily closed using the standard methods, so healing is left to the body's own mechanisms.
The four basic stages of wound healing are these; the times noted are for normal healing and can be much longer for chronic wounds and non-healing wounds:
Phase 1: Hemostasis phase This is the first few hours after an injury or wound. Blood and other fluids leave the body, blood vessels constrict and platelets and other substances clump together near the open wound, forming a fibrin network. That network thickens the blood in the area and releases chemicals sending signals to the surrounding cells.
Phase 2: Inflammatory phase This lasts four to six days and is when immune cells go to the damaged tissue while white blood cells start cleaning the wound out and removing waste.
Phase 3: Proliferative phase It starts once a wound is cleaned out and normally lasts four to 24 days. Several processes occur during this stage to facilitate wound closure, creation of new skin tissue and repair of damaged blood vessels in the area.
Phase 4: Maturation or Remodeling phase It can last from 21 days to two years; the length depends on the presence of infection or excess moisture, your age, nutritional status and other factors. Here, the body creates stronger skin to replace the temporary (granulation) tissue that formed earlier. This is the period of active scar tissue formation.
The Problem of Serious Non-Healing Wounds
Glitches in the wound healing process can occur during any of these stages.
"Wound infections result in a prolonged inflammatory response that interferes with the stage of healing when new tissue is built, contributing to tissue necrosis or death," says Dr. Lisa Derr, medical director of the Jefferson Health Center for Advanced Wound Care and Hyperbaric Oxygen in Cherry Hill, N.J.
"Chronic wounds," Derr adds, "tend to form biofilms — communities of bacteria which are more resistant to typical microbial treatment and which impede healing."
Infected wounds may give off a strong odor, have profuse drainage of pus or other exudates and cause redness, warmth or pain in surrounding areas.
Diabetic foot ulcers can be caused by neuropathy (lack of sensation due to nerve damage), circulatory problems, foot abnormalities and irritation including trauma, friction or pressure. They can occur because diabetics have a reduced ability to fight infection; high blood sugar levels slow down the healing process. Foot ulcers are the precipitating event in more than 80% of diabetic lower leg amputations.
Arterial ulcers, caused by impaired circulation due to cardiovascular disease, may have an inadequate blood supply which leads to poor wound healing. Venous ulcers result from chronically high pressure within diseased veins which damages the skin, disrupts healthy blood flow and increases the risk of infection and cellulitis.
Some dressings for these wounds need to be changed daily; others every few days. Some are impregnated with microbial or antibacterial cream. Cell-based skin substitutes, skin flaps, xenografts with material from a different species and human-donor allografts can be temporary or permanent, depending on the size of the wound and the healing process.
Common Treatments for Non-healing Wounds
Treatment of serious non-healing wounds is often done at a hospital-based or freestanding wound-care clinic and is covered by private insurance or Medicare. Therapies include:
Wound closing technologies such as Vacuum-Controlled Assisted Closure (VAC), which are computer-assisted devices using pressure to increase oxygenation and blood flow while removing wound debris.
The best type of treatment for chronic, non-healing wounds is prevention, especially for people with conditions that predispose them to poor wound healing.
Debridement, which is often done through mechanical or surgical (or both) removal of dead skin using sharp instruments, wound irrigation or surgical procedures
Whirlpool therapy to loosen dead tissue; it's often done before debridement
Cell-based skin substitutes, including grafts made from human placental tissue
Hyperbaric oxygen therapy (HBOT), which is the delivery of 100% oxygen to a patient in a chamber pressurized to more than 1 ½ times the atmospheric pressure at sea level; typically, 20 to 40 treatments are needed, once a day and five times weekly, and each treatment lasts about two hours
Application of specialty dressings, alginates and hydrocolloids to absorb fluid
The best type of treatment for chronic, non-healing wounds is prevention, especially for people with conditions that predispose them to poor wound healing.
In diabetics, foot ulcers can be prevented by keeping blood sugar at healthy levels through proper diet, exercise and medication compliance. Well-fitting shoes should be worn and clean, dry feet should be checked frequently for blistering or ulcerations. Medical care should be sought immediately when needed.
People who are chronically debilitated or with poor nutritional status and relatively immobile, especially those who are bedbound or in a wheelchair, need to shift their weight frequently or be assisted in turning from side to side. Protective padding on elbows and heels can help prevent the development of bedsores.
Wound care in 2021 is much more than the application of a band-aid or gauze bandages. With care and attention, most wounds can be kept free of infection so they can heal in a timely and healthful manner.


