Lower Back Pain? Maybe It's Not Your Back
The problem could be your sacroliliac joint (or S-I Joint). Here are nine steps to relief.
Four years after successful spinal fusion, I began having lower back pain. "This is impossible," I complained to my surgeon. "The bone has successfully fused, and I don't have any discs compressing the nerves coming from my spine."
But the back pain was just as debilitating as the initial problems that led to my surgery. The only comfortable position I found was sitting up in a supportive chair. But have you ever tried to have a good night's rest sitting up in a chair?
"No," he responded. "That's the real clue."
That symptom turned out to be a major clue as to the real problem: my sacroiliac joint, sometimes known as S-I Joint. In fact, according to the National Institutes of Health, the sacroiliac joint is the cause in 25% of people who have reported some incidence of low back pain. Most of that population: older adults who show some degeneration in the joint.
My Doctor Solves the Mystery of My Back Pain
In my case, when I told my orthopedic surgeon, Dr. John Asghar of the Paley Institute in West Palm Beach, Fla., that sitting in a chair stopped the pain, he looked up from the screen showing my CAT scan and had what looked to me a Eureka moment.
He scrolled to the area showing my sacroiliac joint, far to the side of my spine, and saw some potentially problematic areas. On my right side, the joint revealed a bone spur reaching upwards. And on the left, an inflamed area at the top of the joint.
Asghar referred me to a colleague to get an injection of corticosteroids into the sacroiliac joint. At my follow-up meeting two weeks later, I told him that the first hour or two felt great, but then the pain started up again and I was no better off than before. I was disappointed, I said.
"No," he responded. "That's the real clue. The hour or two you felt relief tells us that the numbing medicine took away the pain." And that convinced him his diagnosis was correct. Or at least very likely.
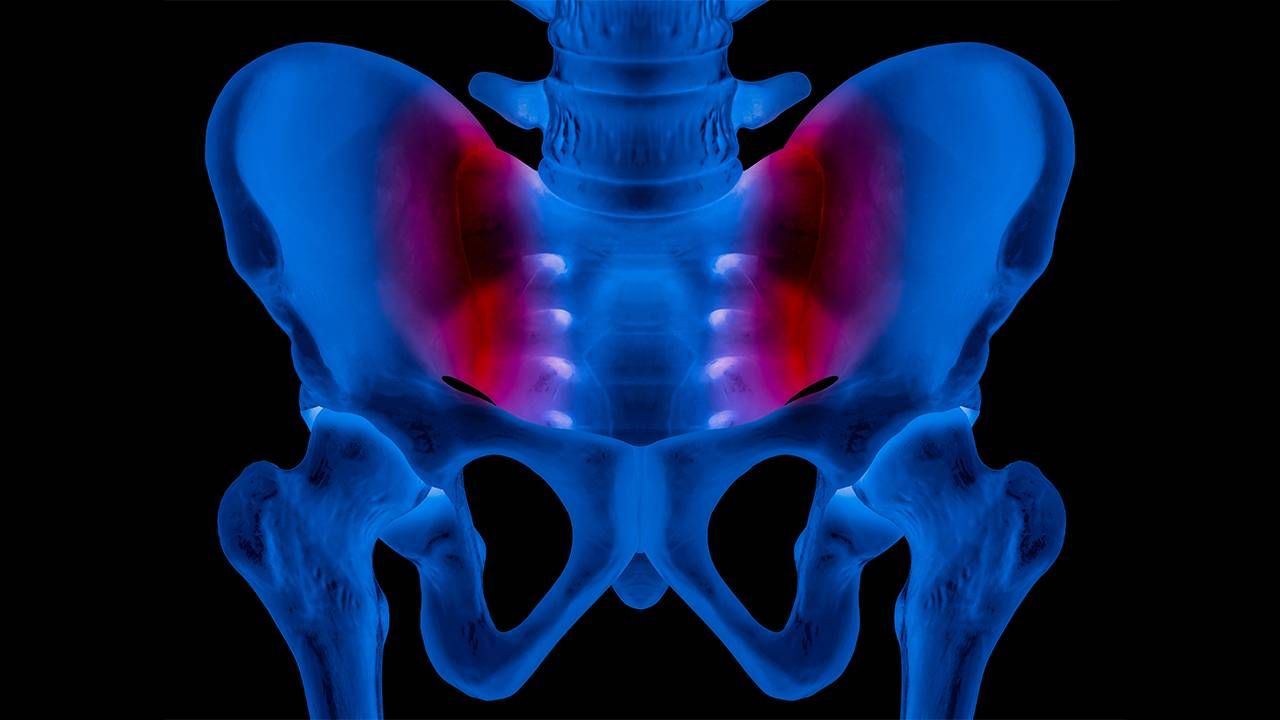
The S-I joint is the largest joint in the body. It connects the sacrum (a bony structure at the base of the lumbar vertebrae) to the pelvis and is held together by ligaments. But unlike most other joints, it is relatively immobile.
Its primary purpose is facilitating weight transfer to and from our legs and upper body, resulting in significant force and stress on the joint. When the ligaments are torn or strained, the joint becomes inflamed, making normal daily activities like bending, walking and even lying in bed difficult. This totally described my symptoms.
With my diagnosis complete, we now began the discussion of the treatment and hopefully, resolution.
9 Steps to Relief From S-I Joint Pain
From what I've learned, below are nine steps to relieve S-I Joint pain. Pain is, of course, completely individual. But most people with S-I joint dysfunction have gotten relief by taking one or more of these steps.
1. R&R: Rest and relaxation can definitely help with any inflammation, even the S-I joint, especially when combined with heat or ice packs near the affected area.
2. NSAIDs: Non-steroidal anti-inflammatory drugs, such as ibuprofen, naproxen or aspirin, can relieve muscle aches and stiffness and reduce swelling and irritation caused by inflammation. But long-term use of them for chronic pain has potentially serious side effects on other organs. So, be sure to check with your physician when taking NSAIDs for an extended period.
Acetaminophen (Tylenol) is not an NSAID and while it does not reduce inflammation, it can be effective in pain relief.
3. Pain medication: Stronger pain medications, such as opioids, must be prescribed by doctors and are extremely effective in relieving S-I joint pain. However, these drugs are controlled substances with severe restrictions.
Long-term use for chronic pain, that is, anything beyond post-surgery, has potentially serious side effects. So, be sure to check with your physician about whether they are right for you.
4. Assistive devices: Ones that reduce the stress on your S-I joint, such as grabbers, walking sticks and canes, shower seats and sock pullers can make activities of daily living easier, giving the joint more time to heal.
An S-I Joint belt, an adjustable strap that wraps around the hip area and provides support to the joint, has shown some limited effectiveness in reducing pain and is available online or at some medical supply pharmacies.
5. Mobility exercise and stretching: Simple, but regular stretching exercises that loosen the quadricep, hamstring and gluteus muscles can help relieve the stress put on the S-I joint. Videos of stretching exercises can be viewed on YouTube by searching for "s-i joint exercises."
6. Physical therapy: Much of what a physical therapist will do will go beyond simply loosening the big muscle groups, providing relief and mobility to the hip and S-I joint. Physical therapy is often most effective when done two to three times per week for several weeks.
Fusion of the S-I Joint is an option for those whose pain is severe and when other steps haven't solved the problem.
7. Corticosteroid injections: Injecting cortisone into the inflamed area is a minimally invasive procedure performed by a physiatrist (physical medicine and rehabilitation doctor) that has achieved some success with joint pain. In some cases, injections can provide relief for several months or longer.
8. Radio Frequency Ablation (RFA): This is another minimally invasive procedure, generally covered by most health insurers and performed by a physiatrist. With RFA, a needle is inserted into the S-I joint and heats a part of the pain-transmitting nerve preventing the nerve from sending pain signals to the brain. The National Institutes for Health says relief has been reported for over 75% of RFA patients and for as long as 10 months.
9. Fusion of the S-I Joint: This is an option for those whose pain is severe and when other steps haven't solved the problem. With sacroiliac joint fusion, the sacrum is grafted to the ilium (the upper part of the pelvis), allowing bone to grow across the joint. This prevents excessive movement in the joint.
The minimally invasive surgery, performed by an orthopedic surgeon, is generally done as an outpatient. While complete fusion can take six months or more, relief generally begins within a few weeks.
The danger with S-I fusion is the possibility that adjacent areas, especially the lumbosacral joint connecting the sacrum to the spinal section, cannot support the additional pressure. That can lead to increased instability in the lower back and more complications.
For more information about these steps, consult your physician.


